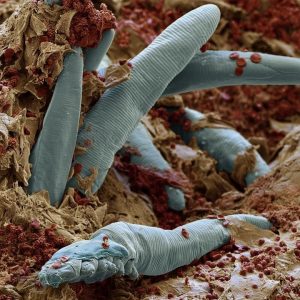
 There are some famous parasites I studied back in my days at the London School of Tropical Medicine & Hygiene (see Loa Loa!), but only recently did I learn that many of us host a common, small parasite on our eyelids which can contribute to dry eyes as well as facial rosacea. My friend and colleague, Dr. Harvey Fishman, wrote about all of this over the summer:
There are some famous parasites I studied back in my days at the London School of Tropical Medicine & Hygiene (see Loa Loa!), but only recently did I learn that many of us host a common, small parasite on our eyelids which can contribute to dry eyes as well as facial rosacea. My friend and colleague, Dr. Harvey Fishman, wrote about all of this over the summer:
Dry eye disease (DED) is far from being a single disease. Rather, it encompasses many different entities. To determine the proper approach to treatment, physicians must differentiate what type of ocular surface disease (OSD) the patient has.1 A host of mechanisms result in various contributing factors.
Regardless of the root cause, as the cornea becomes increasingly irritated it further dries out and normal function deteriorates. Tear production becomes compromised and inflammatory markers appear. If a patient has underlying autoimmune/systemic concerns, the cycle is exacerbated.
Breaking it down: MGD and rosacea
Commonly, patients have DED in combination with meibomian gland dysfunction (MGD) and ocular rosacea.2,3 Because MGD is difficult to treat effectively, nonpharmacological treatments have been explored and are becoming more widely embraced. Intense pulsed light (IPL) is one such powerful solution that not only can treat the lid margins, but also the skin around the eyes that is contributing to the disease as well. IPL has been shown effective in the literature and in my and many other practices.3-13
The mechanism, although not entirely clear, appears to be caused by the reduction of telangietic blood vessels that supply inflammatory factors to the eye. When these pathways are closed, the inflammatory cycle is reduced. In the aesthetic/cosmetic world, IPL has been long known to improve OSD symptoms in facial rosacea patients.
Deeper in the ocular microbiome
Demodex folliculorum is associated with both facial and ocular rosacea. The parasite is a component of MGD, which in turn, is part of DED—it is a vicious cycle. In large numbers, Demodex itself becomes an inflammatory nidus for the eye, consuming bacteria called Bacillus oleronius. It is hypothesized that the interaction of the parasite and the lid’s bacterial load underlies eyelid margin inflammation.14-17
IPL has been shown to dramatically reduce Demodex when studied via punch biopsy before and after treatment. IPL lowers the inflammatory cytokine matrix metalloproteinase 9, a protease that literally ‘eats’ the cornea. Questions remain around the exact mechanism at work and if IPL is definitively killing Demodex—I am in the process of gathering this evidence.
IPL protocol
In my practice, I take a comprehensive ‘holistic’ approach to OSD. I consider everything from the gut microbiome—recommending an anti-inflammatory diet (e.g., omega-3 supplementation)—to devices like IPL and manual expression of the glands to prescription drops to scleral contact lenses for crippling disease.
My IPL protocol using the Optima device (Lumenis) combines those of Laura M. Periman, MD, and Rolando Toyos, MD, plus manual expression and BlephEx/lid debridement to create the “Fishman” Protocol. I treat the entire face, very much like one would for a cosmetic patient, and the upper and lower eyelids. The Optima sapphire-cool light-guide allows me to treat close to the eyelid margin to effectively eradicate Demodex.
Then, I perform manual expression with forceps and grade every single gland. I will use BlephEx (Scope Ophthalmics) or a similar device at the end to clean any dead mites off the lids. I refer to this as “the rub” step like with contact lens hygiene. If necessary, I will perform additional manual debridement. This rigorous protocol takes 20 to 30 minutes.
Conclusion
Patient selection is key for a successful IPL-based treatment. It is indicated for those who clearly have MGD, with evidence of facial and/or lid rosacea. In my experience, for these patients, there is no other technique that can rival IPL.
Dr. Harvey Fishman
References:
- Craig JP1, Nichols KK2, Akpek EK, et al. TFOS DEWS II Definition and Classification Report. Ocul Surf. 2017;15:276-283. doi: 10.1016/j.jtos.2017.05.008.
- Lemp MA, Crews LA, Bron AJ, Foulks GN, Sullivan BD. Distribution of aqueous-deficient and evaporative dry eye in a clinic-based patient cohort: a retrospective study. Cornea. 2012;31:472-478. doi: 10.1097/ICO.0b013e318225415a.
- Dell SJ. Intense pulsed light for evaporative dry eye disease. Clin Ophthalmol. 2017;11:1167-1173. doi: 10.2147/OPTH.S139894.
- Geerling G, Baudouin C, Aragona P, et al. Emerging strategies for the diagnosis and treatment of meibomian gland dysfunction: Proceedings of the OCEAN group meeting. Ocul Surf. 2017;15:179-192. doi: 10.1016/j.jtos.2017.01.006.
- Vigo L, Giannaccare G, Sebastiani S, et al. Intense Pulsed light for the treatment of dry eye owing to meibomian gland dysfunction. J Vis Exp. 2019;1(146). doi: 10.3791/57811.
- Toyos R, McGill W, Briscoe D. Intense pulsed light treatment for dry eye disease due to meibomian gland dysfunction: a 3-year retrospective study. Photomed Laser Surg. 2015;33(1):41-46.
- Viso E, Clemente Millán A, Rodríguez-Ares MT. Rosacea-associated meibomian gland dysfunction—an epidemiological perspective. European Ophthalmic Review. 2014;8(1):13-16.
- Byun JY, Choi HY, Myung KB, Choi YW. Expression of IL-10, TGF-beta(1) and TNF-alpha in cultured keratinocytes (HaCaT Cells) after IPL treatment or ALA-IPL photodynamic treatment. Ann Dermatol. 2009;21(1):12-17.
- Lee SY, Park KH, Choi JW, et al. A prospective, randomized, placebo-controlled, double-blinded, and split-face clinical study on LED phototherapy for skin rejuvenation: clinical, profilometric, histologic, ultrastructural, and biochemical evaluations and comparison of three different treatment settings. J Photochem Photobiol B. 2007;88(1):51-67.
- Prieto VG, Sadick NS, Lloreta J, et al. Effects of intense pulsed light on sun-damaged human skin, routine, and ultrastructural analysis. Lasers Surg Med. 2002;30(2):82-85.
- Karu T. Primary and secondary mechanisms of action of visible to near-IR radiation on cells. J Photochem Photobiol B. 1999;49(1):1-17.
- Farivar S, Malekshahabi T, Shiari R. Biological effects of low level laser therapy. J Lasers Med Sci. 2014;5(2):58-62.
- Gupta PK, Vora GK, Matossian C, et al. Outcomes of intense pulsed light therapy for treatment of evaporative dry eye disease. Can J Ophthalmol. 2016;51(4):249-253.
- Zhang X, Song N, Gong L. Therapeutic Effect of Intense Pulsed Light on Ocular Demodicosis. Curr Eye Res. 2019;44(3):250-256. doi:10.1080/02713683.2018.1536217.
- Fromstein SR, Harthan JS, Patel J, Opitz DL. Demodex blepharitis: clinical perspectives. Clin Optom (Auckl). 2018; 10: 57–63. doi: 10.2147/OPTO.S142708
- Marilyn T Wan1 and Jennifer Y Lin2. Current evidence and applications of photodynamic therapy in dermatology. Clin Cosmet Investig Dermatol. 2014; 7: 145–163. doi: 10.2147/CCID.S35334
- Zhu M, Cheng C, Yi H, et al. Quantitative Analysis of the Bacteria in Blepharitis With Demodex Infestation. Front Microbiol. 2018; 9: 1719. doi: 10.3389/fmicb.2018.01719


