Greetings, TVD friends,
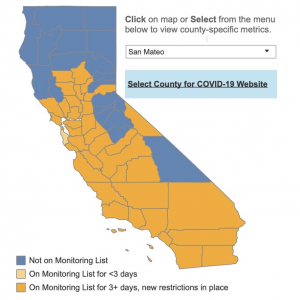
Ugh, so we (San Mateo County) are back on the “watch list”. On Wednesday, July 29th, State officials noted, “San Mateo County is experiencing an elevated case rate that exceeds the State threshold. The County sees roots of community transmission related to social gatherings without sufficient physical distancing and wearing of facial coverings, as well as higher exposure for residents performing work that involves person-to-person contact and crowded housing conditions that make home isolation difficult.” So we continue with our simple message:
- Wear a mask when out in public
- Use “physical distancing” when going out
- Shelter in Place as much as possible
Being back on the State watch list has a number of consequences, the most obvious being the risk of local businesses again being shut down. But right behind that, many anxious San Mateo County parents have just learned that their children’s schools are NOT returning to in-person classes, but rather are staying with “distance learning” for the foreseeable future. I can hear the resounding “ugh”!
So a QUESTION for all of you, really mostly related to all those college students out there. Rather than spending a lot of money on tuition, and then spending your fall quarter at home behind a computer screen, what other creative and life enhancing opportunities are out there? A gap year to explore something you are passionate about? A study abroad experience? A virtual internship? Getting involved with the presidential campaign?
Have you and/or your teen given this some thought, or have some creative ideas? Please email me, and I’ll share our collective experience in these pages.

NOTE: CV🦠News is a labor of love. If you enjoy reading this, please share widely! Was this forwarded to you by a friend? Please subscribe here.

IT’S BEEN 3 WEEKS AND I’M STILL SICK. CAN CORONAVIRUS LAST MORE THAN 2 WEEKS?
Prolonged illness is well described in those patients who require hospitalization for COVID, but what is becoming more and more evident is that some people with relatively mild, but still life-altering symptoms, are not returning to their usual state of health for weeks and even in some cases, months. On July 24, 2020 the CDC released a report looking at this topic and while the study is small and imperfect, the data shows that for many people, COVID symptoms last longer than the expected 2 weeks. One in five previously healthy young adults (age 18-34) were not back to their usual health 14-21 days after testing positive, and one in three of all survey respondents (with a higher percentage in those over 50 years old.) These results are certainly no surprise to those individuals who have become known as “long-haulers” or “long-termers.” “Most people get the virus and after a few weeks their symptoms resolve,” said Dr. Robert Glatter, emergency physician at Lenox Hill Hospital in New York City. “We’re seeing a different spectrum where people don’t recover, and they have symptoms from weeks to months.”
No one knows exactly why this happens, but Akiko Iwasaki, an immunologist at Yale, offers three possibilities: “Long-haulers might still harbor infectious virus in some reservoir organ, which is missed by tests that use nasal swabs. Or persistent fragments of viral genes, though not infectious, may still be triggering a violent immune overreaction, as if “you’re reacting to a ghost of a virus,” Iwasaki says. More likely, the virus is gone but the immune system, having been provoked by it, is stuck in a lingering overactive state.” In fact, Glatter has said “we’re learning that these long-haulers are a population that often test negative. Some of these patients have never had a positive test,” implying that their diagnoses were made on a clinical basis given that the symptoms weren’t necessarily bad enough to warrant testing when tests were still limited.
The most common long-term symptoms are fairly non-specific and include ongoing fatigue and muscle aches, although some patients have reported prolonged daily fevers, persistent nighttime chills, breathlessness and some also have strange neurologic symptoms “brain-fog, hallucinations, delirium, short-term memory loss, or strange vibrating sensations when they touch surfaces.” Social media has connected many of these long-haulers in support groups, which patients find very helpful for coping. In a report generated by one such support group (Body Politic on Slack with 4000 people that have had symptoms for over 30 days and often double that), one author said “the symptoms wax, wane, and warp over time. It really is a grab bag…Every day you wake up and you might have a different symptom.”
We know that having more severe disease or chronic conditions makes people more likely to have long term effects, but of the otherwise healthy people that get COVID, we don’t know what makes one person more likely than another to have prolonged symptoms. Thus, the takeaway is yet again the following: wash your hands, wear a mask, and keep your distance from others.
Sources: The Atlantic and USA Today.
 WE HEAR A LOT ABOUT COVID “MORTALITY”, SHOULDN’T WE BE TALKING ABOUT COVID “MORBIDITY”?
WE HEAR A LOT ABOUT COVID “MORTALITY”, SHOULDN’T WE BE TALKING ABOUT COVID “MORBIDITY”?
We are familiar with the stats: 80% of those infected with SARS-CoV-2 will have mild or asymptomatic disease, while 20% will need to be admitted to the hospital for oxygen support, and 5% of those will be admitted to intensive care units for breathing support (sometimes mechanical ventilation).
Most studies to date have appropriately focused on the mortality of COVID-19 (what percentage of those infected die of the disease), but only one has focused on the longer-term outcomes (morbidity) of those who have a mild or moderate disease. Because this virus can cause dysregulation of the immune system, sometimes inflammation so severe it is termed a “cytokine storm,” it can affect the functioning of organs all over the body and in the small blood vessels leading to them which can clot and cause damage to the kidney and heart.
While we might expect survivors of severe disease to have long-lasting consequences, it seems COVID-19 can cause persistent symptoms even in those with milder illness. First-person accounts are all over Slack and Facebook, many still suffering more than 60 days after infection. They call themselves “long-haulers” or “long-termers.”
A well known, credible long-hauler is Paul Garner, an infectious disease professor at the Liverpool School of Tropical Medicine in the UK, infected in late March. In a blog post published by the British Medical Journal he describes having:
“. . . muggy head, upset stomach, tinnitus (ringing in the ears), pins and needles, breathlessness, dizziness and arthritis in the hands.”
These symptoms have waxed and waned but not yet resolved. He says this is:
“. . . deeply frustrating. A lot of people start doubting themselves . . . Their partners wonder if there is something psychologically wrong with them.”
To date, only one peer-reviewed study has looked at the long term symptoms of COVID-19 infection: a single group of 143 survivors from Rome. Most did not require hospitalization and all were assessed 60 days after infection. 44% of them reported a worsened quality of life, including persistent fatigue (53%), breathlessness (43%), joint pain (27%), and chest pain (22%).
The COVID-19 pandemic is still in its early days and we clearly have much more to learn about the disease and its aftermath. Survivors with persistent symptoms, the “long-haulers,” are clearly not uncommon and we have many lessons to learn. Perhaps the most fundamental one? Do your best not to get infected with COVID-19 in the first place.
Above all: WEAR A MASK IN PUBLIC AREAS!
Stay home if you are sick, wash your hands, reserve testing for those who might be infected when testing capacity is limited, and be honest with those in your household and social bubble (Quaranteam) about potential exposures.
 CAN COMMON HEARTBURN MEDICINE INCREASE MY RISK FOR COVID19?
CAN COMMON HEARTBURN MEDICINE INCREASE MY RISK FOR COVID19?
Proton pump inhibitors or “PPIs” (such as omeprazole/Prilosec and esomeprazole/Nexium), a common class of acid-reducing medications available by prescription and over the counter, work by turning off the pumps in cells that release acid into the stomach. They are commonly used as a treatment for gastroesophageal reflux disease (GERD), gastritis or ulcers, and can be taken once or twice a day. Although the impact of acid suppression on SARS-CoV-2 is unknown thus far, prior data has revealed that SARS-CoV-1 infectivity is impaired in a more acidic environment (pH <=3), the normal pH of a healthy stomach, whereas less acidic pH in the range achieved with PPI therapy does not inactivate the virus. In a July study published in pre-print form in the American Journal of Gastroenterology, Dr. Brennan Spiegel at UCLA and his team of scientists conducted an online survey of over 50,000 people with a history of reflux symptoms, in which 3,386 (6.4%) reported a positive COVID-19 test. In a regression analysis, which helps scientists to control for a wide range of confounding factors, the scientists found that individuals using PPIs up to once daily had a 2x likelihood for reporting a positive COVID-19 test when compared to those not taking PPIs, and those taking PPIs twice daily had a 4x likelihood of reporting a positive COVID-19 test. This was not true for other acid-reducing medications like H-2-receptor blockers (Pepcid/famotidine). “This study does not mean that people on PPIs should just stop their medicines,” says Dr. Spiegel. “PPIs work and, in most cases, their benefits outweigh the risks. As always, the decision about whether, when, and how to modify PPI dosing should be based on a thoughtful assessment of the risk-benefit ratio for individual patients. As with any medication, the lowest effective dose should be used when clinically indicated, and, when appropriate and consistent with best-practice guidelines, H2RAs may also be considered as an alternative treatment for acid-related conditions.”
 DO YOU FIND YOURSELF BAKING DURING THE PANDEMIC?
DO YOU FIND YOURSELF BAKING DURING THE PANDEMIC?
Since the start of the pandemic, grocery aisles were being emptied and some of the top ingredients were flour, butter and yeast. On first pass this makes perfect sense, these are pantry staples and people feared shortages.
Very quickly though, a different phenomena was apparent, everyone was baking bread, cookies, cakes, croissants, and a french pastry recipe that takes 4 days to prepare. The natural question is why did “stress baking”, as it is now referred to, become so popular?
For centuries, baking, in particular bread, has been a daily practice among most cultures. It provides predictability to meals and represents a time to come together to eat. During this time of massive uncertainty, baking provides a distraction, comfort and something to look forward to. Our brain craves order when there is disorder. A recipe provides a wonderful step-by-step approach to a pleasurable result. In addition, the pandemic has forced an unnatural solitude and restrictions on gatherings. Food brings people together, whether it is cooking together, eating together or sharing recipes. Instagram and Facebook have seen a surge in recipe sharing.
I know for myself, cooking and baking have always been a cherished hobby. During the pandemic, my family like many others have been baking more than ever and attempted to make vegan pavlova which I had never even heard of before March. Find the recipe here.
So if you are interested in trying out some great desserts, I’m sharing my apricot-berry crumble recipe here which my daughters and I have made at least 20 times. It’s easy, delicious and will get you started on your own baking tradition.
If you are interested in making your own sourdough bread (it takes 4 days), then this is the best recipe on the internet.
As we continue our new normal, enjoy the pure joy of creating something from start to finish and fill your kitchen with all of the soothing aromas of cinnamon, nutmeg and cardamom.

HOPE AND GRACE
If you have made it this far, time for a reward, something to lighten your day, and acknowledge the human spirit. Find some escape, or perhaps even inspiration, in this collection of works and perspectives gathered from around the world. Please contact me directly if you have come across something that has lifted your heart today. Dr. Eric Weiss
Antibodies (Do You Have The) [Music Video]. Worth a watch and listen for a smile! Emmy-nominated actor Nicholas Braun — a.k.a. Cousin Greg from Succession, wrote the lyrics and then crowd-sourced the music. From Nick, “Thanks to everyone who sent me their videos these last couple months. YOU inspired this awesome, creative project. I got to connect with so many talented singers, producers, guitarists, pianists, and artists of all sorts – just making stuff in their bedrooms and basements. I hope this track and this video brings you as much joy as it did for me to make it.”

A Pandemic Poem-Prayer. Phyllis Cole-Dai is a writer and poet, perhaps best known for ‘The Emptiness of Our Hands’. On her 58th birthday earlier this year, she wrote 58 one-line pandemic prayers and crafted them into a poem. See the text here. Perhaps it will give you a boost. You can listen to Phyllis read the poem here or download it here.
Again, CV🦠News is a labor of love. If you enjoy reading this, please share widely! Was this forwarded to you by a friend? Please subscribe here.
*****
Yours, in health and resilience,
Eric and the TVD MD team…